
Trauma can have a large impact on all aspects of a person’s life including how they interact with community services. (See What is Trauma? and The impact of trauma.) Trauma-informed practice is thus an important foundation for services and practitioners in a range of settings. The first approaches to “treating” trauma were in response to military personnel who had fought in wars,[1] but gradually there was a greater recognition of trauma caused by sexual violence, domestic and family violence, childhood abuse and neglect, and other forms of trauma. As Judith Herman[2] demonstrated in her seminal work Trauma and Recovery (which explored the trauma many women experience in the home), trauma is not simply the result of rare, extreme events, but is much more common than war.
Psychological trauma is an affliction of the powerless. At the moment of trauma, the victim is rendered helpless by overwhelming force. When the force is that of nature, we speak of disasters. When the force is that of other human beings, we speak of atrocities. Traumatic events overwhelm the ordinary systems of care that give people a sense of control, connection, and meaning.
It was once believed that such events were uncommon. … Rape, battery, and other forms of sexual and domestic violence are so common a part of women’s lives that they can hardly be described as outside the range of ordinary experience. …
Traumatic events are extraordinary, not because they occur rarely, but rather because they overwhelm the ordinary human adaptations to life. Unlike commonplace misfortunes, traumatic events generally involved violence and death. They confront human beings with the extremities of helplessness and terror, and evoke the responses of catastrophe. (p. 33)
As the nature of trauma became better understood, approaches to supporting people with trauma began to change. Susan Salasin[3] argues that, rather than clinical treatment of symptoms or psychosocial education and empowerment models, trauma-informed practice now:
Changes the opening question for those seeking services from “What is wrong with you?” (patient or consumer) to “What has happened to you?” (survivor). Trauma-informed care is initiated by assumption that every person seeking services is a trauma survivor who designs his or her own path to healing, facilitated by support and mentoring from the service provider. (p. 18)
According to the Blue Knot Foundation,[4] trauma-informed practice:
- Rests on the foundation principle of “do no harm.”
- Does not require clinical knowledge and is not “treatment.”
- Understands the effects of stress on the brain and body.
- Considers what has happened to the person (not what is “wrong” with the person).
- Regards “symptoms” as outgrowths of coping strategies.
- Is sensitive to client comfort levels and to THE WAY IN WHICH a service is delivered (not just WHAT the service is).
- Works with (rather than “doing to”) the client. (p. 1)
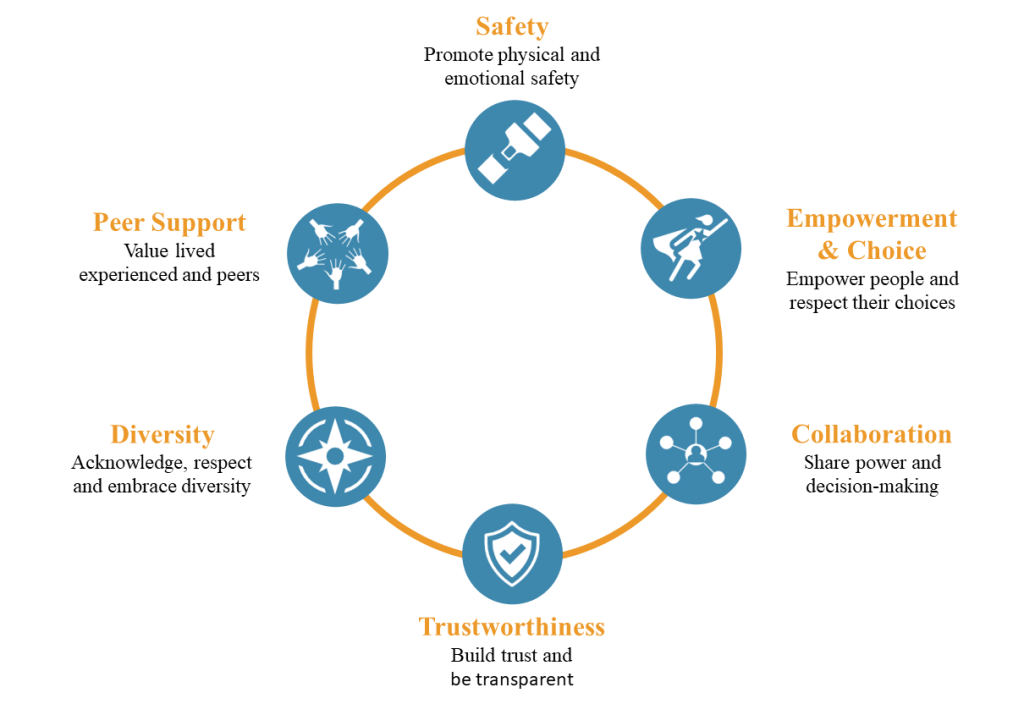
Drawing on the NSW Agency for Clinical Innovation,[5] the Blue Knot Foundation[4] and the Substance Abuse and Mental Health Services Administration[6] we can identify six broad principles of trauma-informed practice (see figure below):
- Safety – Promote physical and emotional safety
- Empowerment & Choice – Empower people and respect their choices
- Collaboration – Share power and decision-making
- Trustworthiness – Build trust and be transparent
- Diversity – Acknowledge, respect and embrace diversity
- Peer Support – Value lived experienced and peers
Each of these six principles are discussed below.
Continue reading










